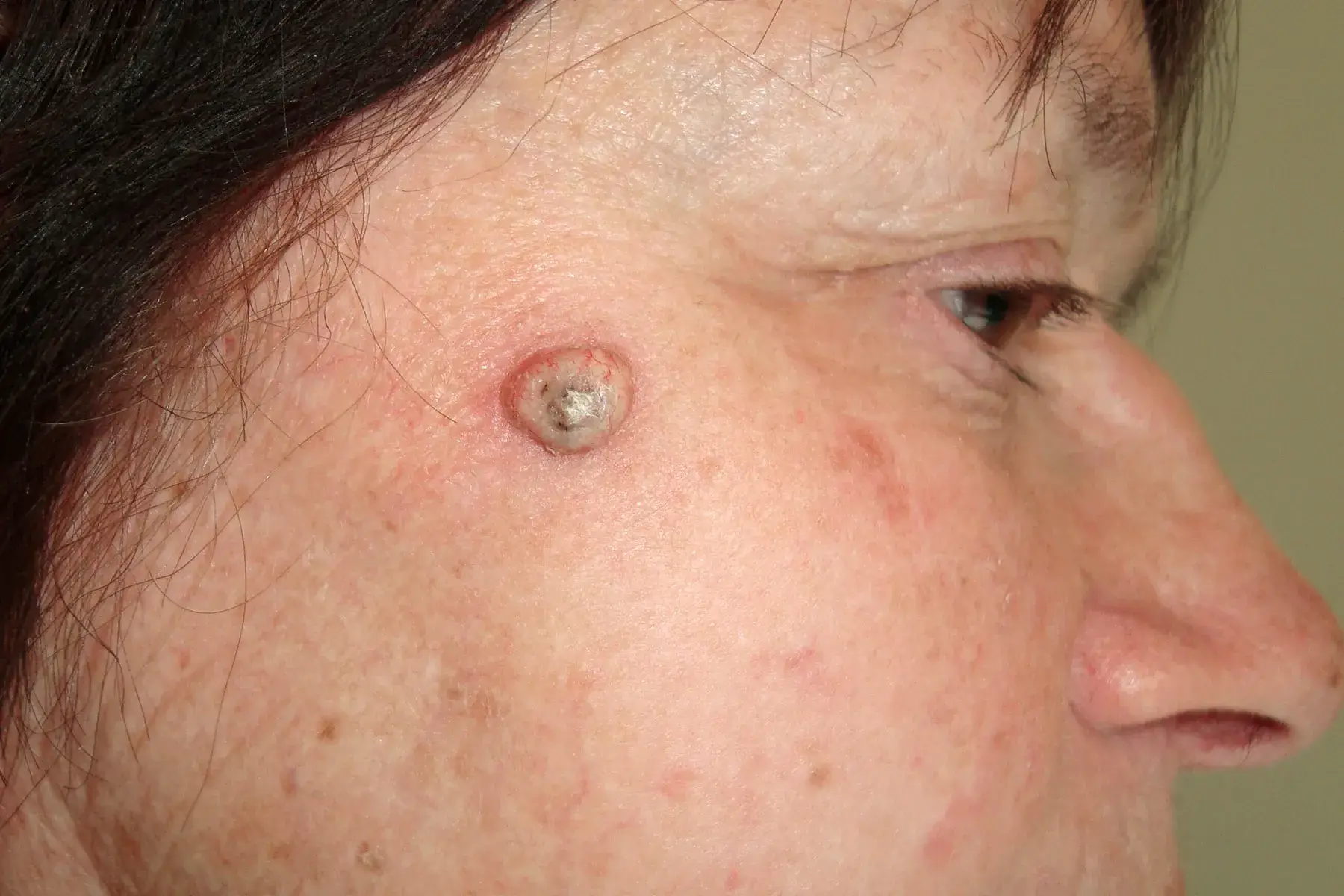
Overview
Squamous cell carcinoma is the second most common skin cancer, accounting for about 20% of skin cancer cases. Unlike basal cell carcinoma, SCC has greater potential to spread to lymph nodes and distant organs, making early detection and appropriate treatment essential. With early detection and proper treatment, cure rates exceed 95%. Regular skin screening and sun protection are critical for prevention and early diagnosis.